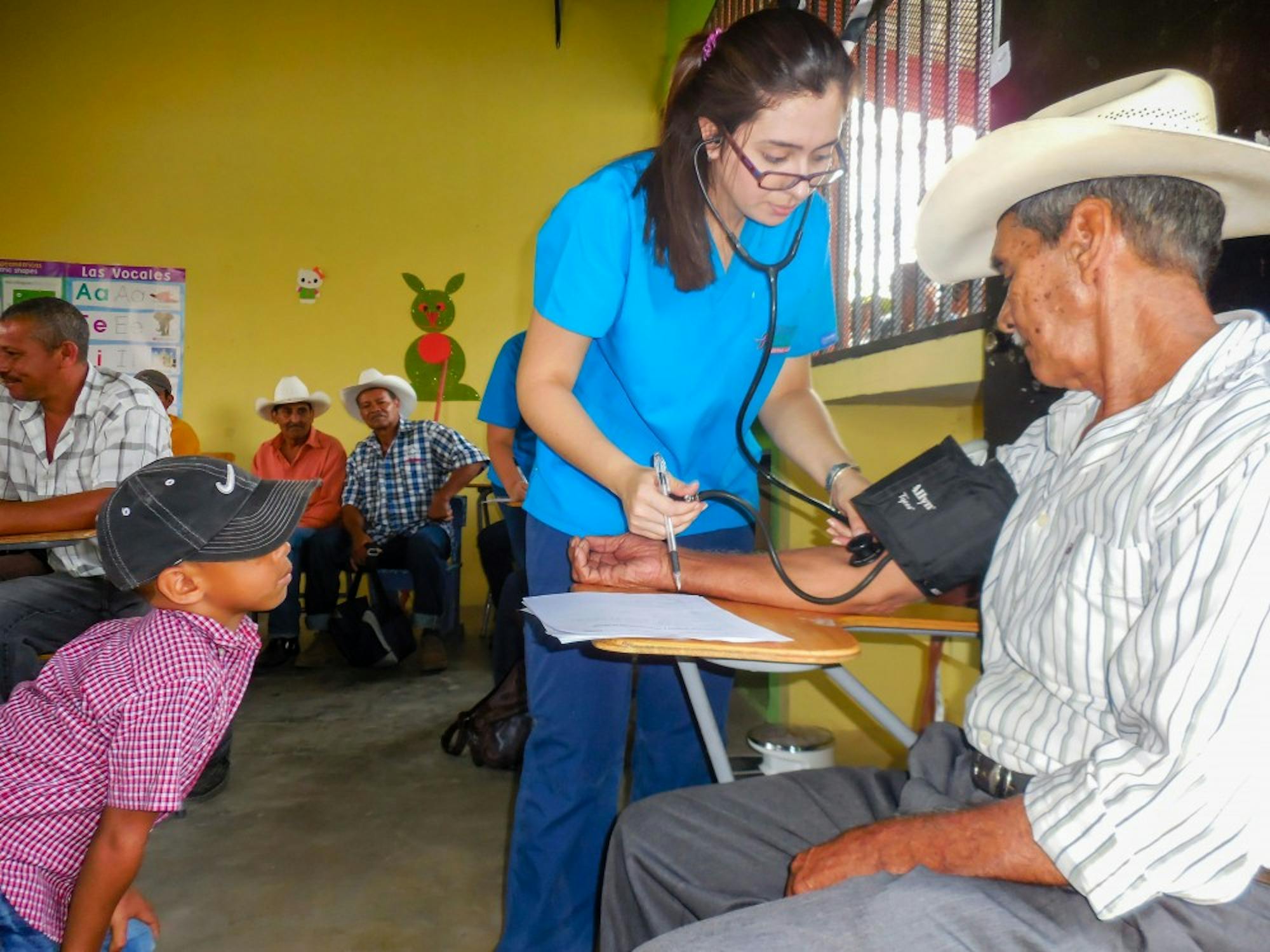
Since 2011, researchers at the Geisel School of Medicine and Dartmouth-Hitchcock Medical Center have been conducting projects in Honduras that help citizens who lack medical care, in addition to furthering academic understanding of cancer there. This past winterim break, Dartmouth students also traveled to El Rosario, a rural village in Honduras, to educate Honduran teenagers on leadership and public health concerns with non-profit Americans Caring Teaching Sharing Honduras.
Linda Kennedy, the associate director of community affairs at the Norris Cotton Cancer Center who helped spearhead the research, was not a stranger to Honduras: For about 12 years, she has served citizens of rural Honduras through ACTS. With this Norwich-based organization, she worked to address public health concerns and community building in rural areas by facilitating a program called La Fuerza para el Futuro, which is a leadership program for teenagers in rural Honduras and translates to “The Force for the Future,” in a rural village.
In 2011, she approached Greg Tsongalis, a Geisel professor of pathology and laboratory medicine, with the idea of establishing a medical research aspect of the College’s work in Honduras. Since then, they have begun conducting ongoing projects together, which fall under the umbrella of DHMC’s Community-Led Action Research in Oncology, or CLARO, a program which emphasizes the importance of addressing community needs through research.
“[With CLARO], we take the ideas for the research projects from what Hondurans need,” Kennedy said. “They’re our partners. Our scientists come up with the methods but concerns arise from the community.”
Tsongalis echoed the importance of furthering medical research while also providing much-needed care for Honduran citizens.
“We wanted to do something that would be both scientifically and medically interesting but also really help the people in these villages in Honduras and be sustainable,” he said.
One of the largest points of focus for the College’s research in Honduras is cancer, particularly the prevalence of cervical cancer in Honduran women. In developing countries like Honduras, women lack access to the human papilloma virus, or HPV vaccine, Pap smears and cervical cancer treatments. Nationwide, Honduras has the second-highest rate of cervical cancer in Latin America.
According to Kennedy, it is “a public health disaster” with a devastating effect on Honduran families.
“For every woman [who] dies of cervical cancer in a low-income country, there’s at least a handful of children who don’t have a mother,” she said, adding that cervical cancer is “a wholly preventable disease.”
To address this concern, researchers and volunteers have opened two women’s health clinics in rural Honduras and have been successful in screening hundreds of women for cancer.
“We say that 40 to 50 percent of cancer is preventable, but it’s not preventable in [low- and middle-income] countries because it’s preventable by life choices and screening.” Kennedy said. “As it turns out, people in those countries aren’t aware of those choices and they don’t have access to screening.”
Nearly all cases of cervical cancer occur when women contract HPV. In developed countries like the U.S., there is wide access to the HPV vaccine. Additionally, women in the U.S. undergo regular Pap smears to check for cervical cancer and potentially malignant cells. If malignant cells are spotted and treated early, the cancer is usually treatable, but the same is not true for cancer identified in more advanced stages.
In spring 2017, after men in rural Honduras requested the same kind of testing that women received, the research group hosted its first cancer screening clinic for men, according to Tsongalis.
In the clinics, researchers utilize low-tech methods to screen for cancer and based on those results, the medical personnel determine which patients need high-tech screening through Liga Contra el Cancer, the partner cancer center located in San Pedro Sula.
Due to the success of these clinics, Tsongalis hopes to continue hosting them for men and women biennially.
This year, researchers broadened the reach of their work to include urban Honduran areas, such as San Pedro Sula, as they hosted a clinic to screen for high risk HPV at a factory with 2,000 women. Researchers are working on developing an improved method for reviewing the samples obtained from this kind of clinic.
Researchers have also established a program to offer chemotherapy patients palliative care through phone calls. When experiencing pain and side effects of their diseases and treatment, cancer patients can call trained nurses in Honduras for advice about pain and symptom management. This kind of care allows patients to remain strong enough to finish their cancer treatment.
An additional CLARO project investigated the potential for farmers’ exposure to agricultural products like pesticides and herbicides, many of which are outlawed in the U.S., for causing cancer.
To conduct this research, College faculty used a technique developed by Thayer School of Engineering doctoral candidate Ethan LaRochelle. The team added a harmless fluorescent tracer to the chemicals that farmers were spraying in the fields. After the farmers finished working, researchers took pictures of their chemical-covered hands in a UV light box that LaRochelle designed. The images were then processed using LaRochelle’s algorithm to identify the areas on the hands that were most covered by the chemical.
In addition to LaRochelle, other students, especially those from Geisel, have been crucial to facilitating and developing the projects in Honduras, Kennedy added.
CLARO and the researchers’ work to help qualified medical professional in their analysis of samples obtained from cancer screenings. This is significant because there are only a handful of pathologists in the entire country. Due to this development, Tsongalis and his team are now working to establish a telepathology system with a cancer center in Honduras, where the medical personnel in Honduras would prepare the samples on slides and then send electronic images of them to College researchers in the U.S. for future analysis, potentially aiding the timely treatment of cervical cancer and preventing backlog.